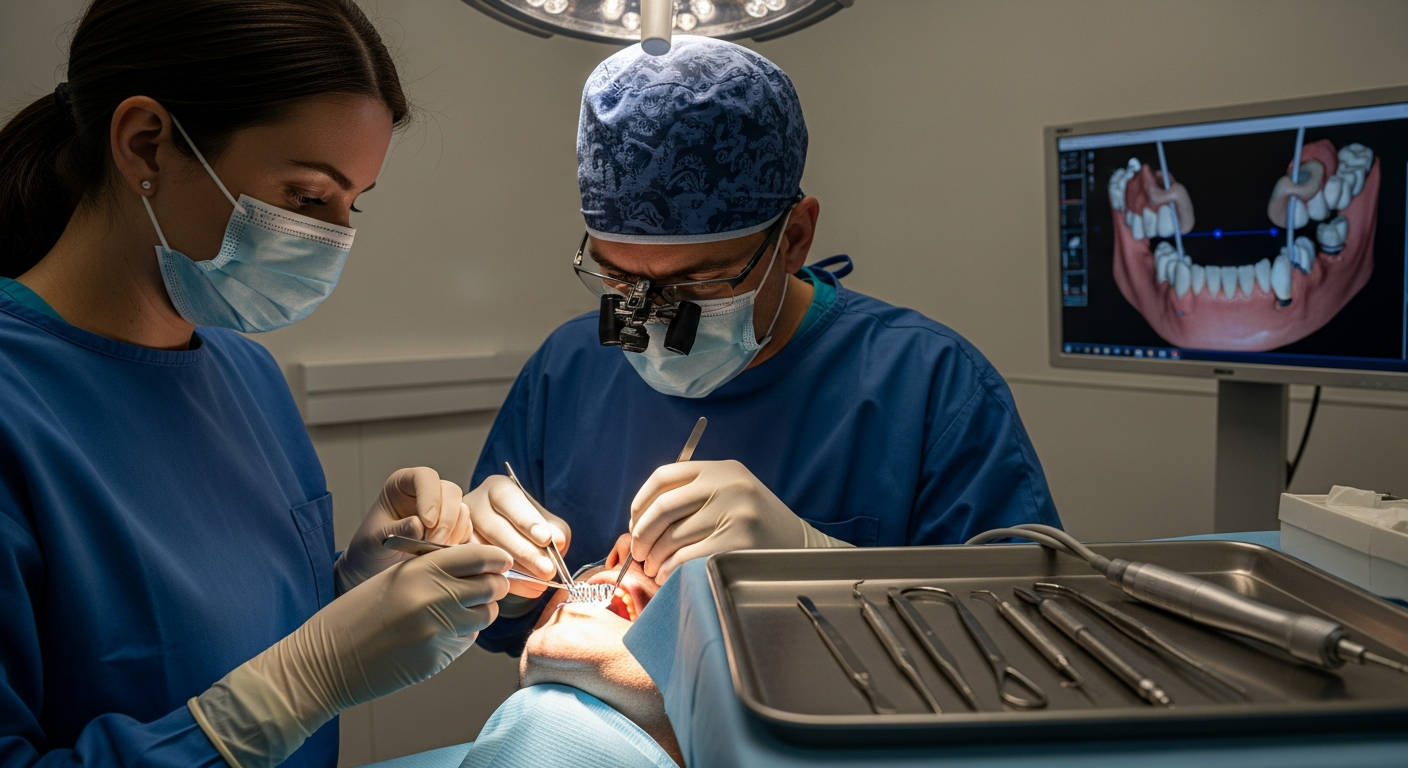
How to apply for dental implants on the NHS
Applying for dental implants through the NHS requires meeting strict clinical criteria and following a defined referral process. Understanding how assessments are conducted, what medical conditions are considered, and which documentation may be needed helps applicants prepare effectively. This guide explains each step of the application pathway, from initial consultation through specialist evaluation, along with expected waiting times and the role of NHS funding decisions. Alternatives available if NHS treatment is declined are also outlined, giving seniors a clearer overview of their options.
Access to dental implants on the NHS in the UK tends to be tightly controlled because implants are complex, resource-intensive treatments. In many areas, they are reserved for patients whose oral health, function, or wellbeing is significantly affected, and where other standard NHS options are not suitable.
NHS eligibility criteria for dental implants
NHS eligibility criteria for dental implants focus on clinical necessity. In practice, this often means implants are considered when tooth loss is linked to trauma, cancer treatment, congenital conditions (for example, missing teeth from birth), or severe medical complications that make conventional dentures difficult or unsafe. Significant functional impairment, such as difficulty chewing or speaking that cannot be reasonably managed with other treatments, can also be relevant.
It is also common for eligibility to depend on whether your mouth is healthy enough for implant surgery and long-term maintenance. Factors such as uncontrolled gum disease, smoking, poorly managed diabetes, or very limited bone support may affect suitability and the likelihood of approval, because implants require stable oral health and ongoing hygiene.
Even when there is a genuine need, availability can vary between local NHS commissioning arrangements. That means two patients with similar circumstances may experience different pathways depending on where they live and which services are commissioned locally.
Referral steps for applying through the NHS
Referral steps for applying through the NHS usually begin with a consultation at your general dental practice. Your dentist will assess your oral health, discuss symptoms and functional problems, and review what treatments are appropriate within NHS care. In many cases, you may first be offered conventional options such as partial dentures, full dentures, bridges, or other restorative approaches that are more routinely available.
If your dentist believes implants might be clinically justified, they can refer you to a service such as a hospital oral and maxillofacial unit, restorative dentistry department, or an NHS community dental service pathway, depending on your circumstances. The referral typically summarises your history, current problems, and why alternative treatments may be unsuitable.
After referral, you may be invited to a specialist assessment appointment. This is often where the decision-making becomes more formal: the specialist team evaluates implant suitability, checks whether NHS criteria are met, and determines whether funding approval is required before any treatment can proceed.
Medical documents needed for implant assessment
Medical documents needed for implant assessment help the specialist team understand both your dental situation and your general health risks. You will typically need up-to-date information about your medical history, regular medications, allergies, and any long-term conditions that affect healing, bleeding risk, or infection risk.
Dental records matter as well. Recent dental examinations, gum (periodontal) assessments, and dental X-rays are commonly used to evaluate bone levels and oral health stability. In some cases, additional imaging such as a CT scan may be requested to assess bone volume and anatomical structures before confirming whether implants are feasible.
If your tooth loss is connected to a wider medical event, supporting clinical letters can be important. Examples include documentation linked to head and neck cancer care, facial trauma, congenital diagnoses, or conditions that make wearing dentures particularly difficult. Having clear, consistent evidence can make the assessment process smoother and reduce delays caused by missing information.
Waiting times and funding decisions explained
Waiting times and funding decisions explained: once you are referred, timelines can vary widely depending on local demand, specialist capacity, and whether funding approval is needed. Some patients are assessed relatively quickly but then wait longer for scans, planning appointments, or surgery slots. Others may experience longer waits before the initial specialist consultation.
Funding decisions are usually based on whether the case meets the required threshold for NHS implant treatment in your area and whether the proposed plan is clinically appropriate. Some implant pathways require prior approval from local NHS commissioners, while others are managed within hospital service criteria. You may be told that implants are clinically possible but not funded under local rules, which can be frustrating but is not uncommon.
If you are awaiting a decision, it can help to ask what the next step is and what information is still needed. Keeping routine dental care up to date during the waiting period is also important, because active decay or gum disease can affect both clinical suitability and the willingness of services to proceed.
Alternatives if NHS implant treatment is declined
Alternatives if NHS implant treatment is declined often include treatments that can still restore function and appearance effectively. Dentures remain a standard NHS option and can be improved with careful design, relines, or adjustments. Bridges may be suitable in some cases, depending on the condition of neighbouring teeth and bite stability.
If the main issue is discomfort or poor retention of dentures, your dentist may be able to explore changes in fit, materials, or bite balance. Sometimes the challenge is not the concept of a denture itself, but whether it has been optimised for your mouth and whether gum and bone changes have been addressed.
Some people consider private implant treatment after an NHS decline. If you go down that route, it is sensible to request a clear written treatment plan, ask what maintenance will be required long-term, and ensure you understand what happens if complications occur. Whether treatment is NHS or private, implants need ongoing checks and excellent home care.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
In summary, applying for dental implants on the NHS usually requires a clinically significant reason, a dentist-led referral, and specialist assessment against local funding rules. Preparing the right medical and dental information, understanding why decisions take time, and knowing the realistic alternatives can help you navigate the process with clearer expectations.